Diabetic foot ulcer debridement | Podiatrist Brisbane Woolloongabba
Foot ulcers due to diabetes can be very difficult to heal without an expert understanding of the role of weight-bearing pressure, wound healing physiology, blood flow and sensation in the diabetic foot. Diabetic foot ulcer debridement is a cornerstone in the management of these difficult wounds.
In our practice, we have a particular focus on healing foot ulcers due to the combined effects of peripheral neuropathy, peripheral arterial disease and diabetes. Our practice has had a long standing association with the Queensland Diabetes Centre at the Mater Hospital for over a decade, and our podiatrists have significant experience in the assessment and management of diabetic foot complications.
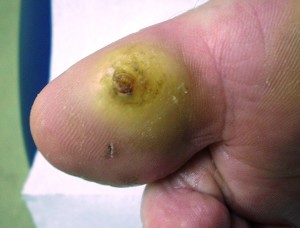
The medical and scientific literature is very clear about the importance of sharp or surgical wound debridement as a basic tenant of wound healing for chronic diabetic foot ulcers. This is especially the case for neuropathic ulcers – caused by a lack of sensation.
Without removable of callused, necrotic or non-viable (dead) tissue, it is extremely difficult to heal most foot ulcers. However, this approach needs to be coupled with adequate pressure offloading (removable cast walkers, casts or orthotics) in order to allow the underlying tissues to then heal back to full skin integrity.
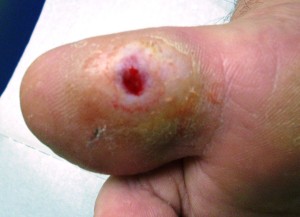
Debridement is usually a painless process, especially if peripheral neuropathy is present. Following sharp debridement, some bleeding may occur for a short time, after which the foot is dressed and bandaged to protect these fragile tissues.
If you are having problems with a chronic non-healing diabetic foot ulcer, contact us immediately for help.