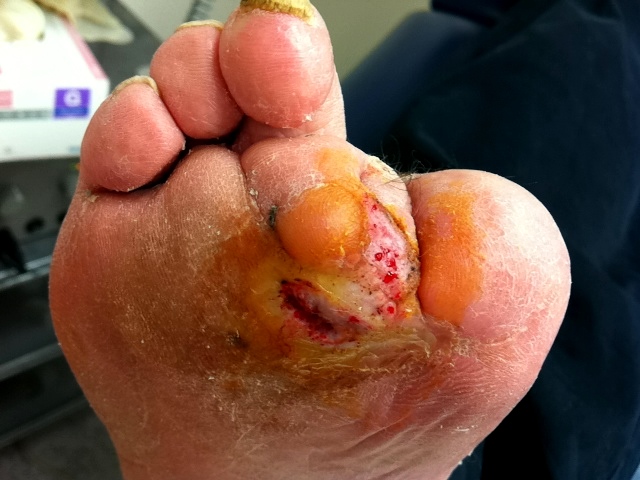
Diabetic Foot Treatment - Our Brisbane Podiatrists are experts in diabetic foot complications
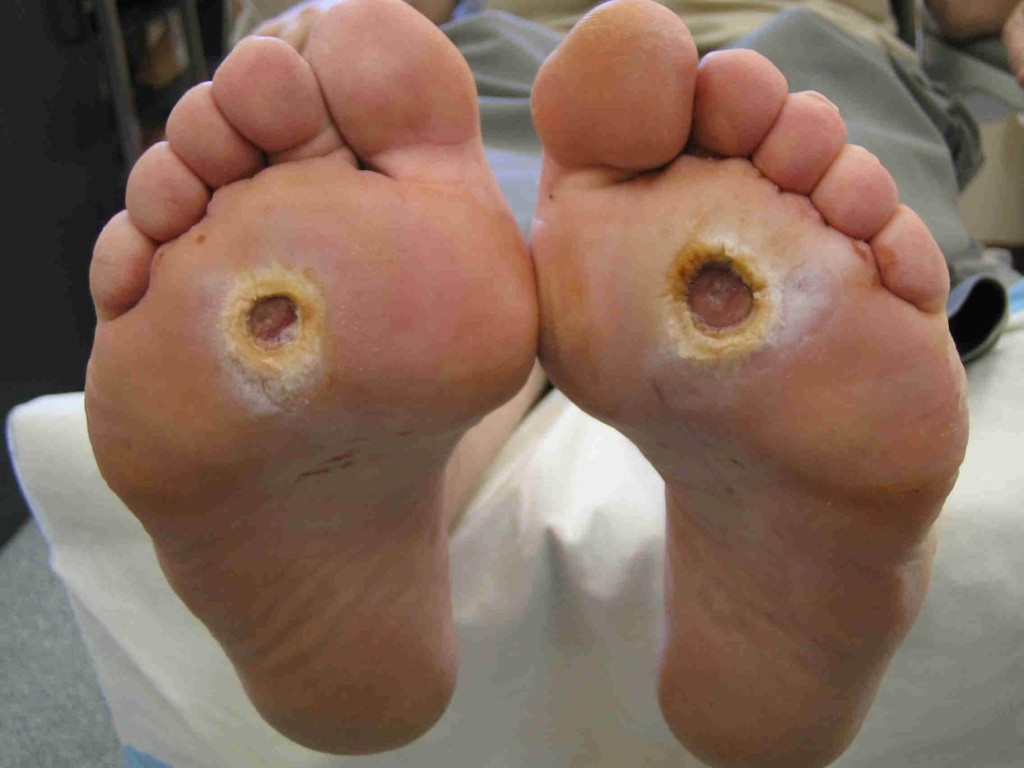
Do you have a foot complication or foot ulcer from diabetes? Our team can help.
Diabetic foot complications are a special interest area for our practice. We have extensive knowledge and expertise in this area. Diabetic foot complications are a serious problem that can lead to limb loss and amputation.
Diabetes causes two main complications in feet.
People with diabetes are at risk of developing ulceration and infections in their feet, which have the potential to lead to amputation of the foot or leg. Even trivial or minor injuries have the potential to become very serious and threaten a limb.
Peripheral Neuropathy
This is a condition where there is damage to the nerves in the extremities, usually feet more than hands. This can lead to a loss of sensation, or chronic nerve pain.
Peripheral Arterial Disease
This is a condition where there is narrowing or blockages in the main arteries that carry blood from the heart down to the foot. Diabetes can also affect the tiny blood vessels in the foot (microvascular disease).
Foot complications are the most common cause of a hospital admission for a person with diabetes.
Health professionals recommend an annual diabetic foot check-up and review for all people with diabetes.
Foot care tips for people with diabetes
- Inspect your feet on a daily basis for any new injuries, cuts or unusual discolouration
- See your podiatrist or GP/specialist immediately if you suspect a problem
- Have an annual foot check-up with your podiatrist
- Take care of your blood glucose levels, it lessens the risk of foot complications
- Don’t walk outdoors without footwear, it lessens the risk of injury
- Don’t try to treat simply problems like corns, calluses or ingrown toenails yourself, this can lead to serious harm
- Buy well fitting shoes with plenty of room. If you have peripheral neuropathy you might not be able to tell if the shoe fits well.
Charcot Foot
One of the lesser known, but most devastating, complications of diabetes is known as a Charcot neuroarthropathy (or a Charcot joint). The name is derived from a French physician, Dr Jean-Martin Charcot, who first identified this condition in patients with peripheral neuropathy (in this case, due to syphilis) whilst working in Paris in the 1800’s.
Charcot neuroarthopathy is a situation where one or more joints within the foot can ‘collapse’ and cause serious deformity and instability, often after a seemingly trivial or inconsequential injury. The foot can change appearance quite dramatically over the course of a few months, and it is difficult to diagnose at first – as it is often confused with infection or gout. Long term, patients with a Charcot joint can be left with a severely deformed foot and high risk of ulceration or amputation.
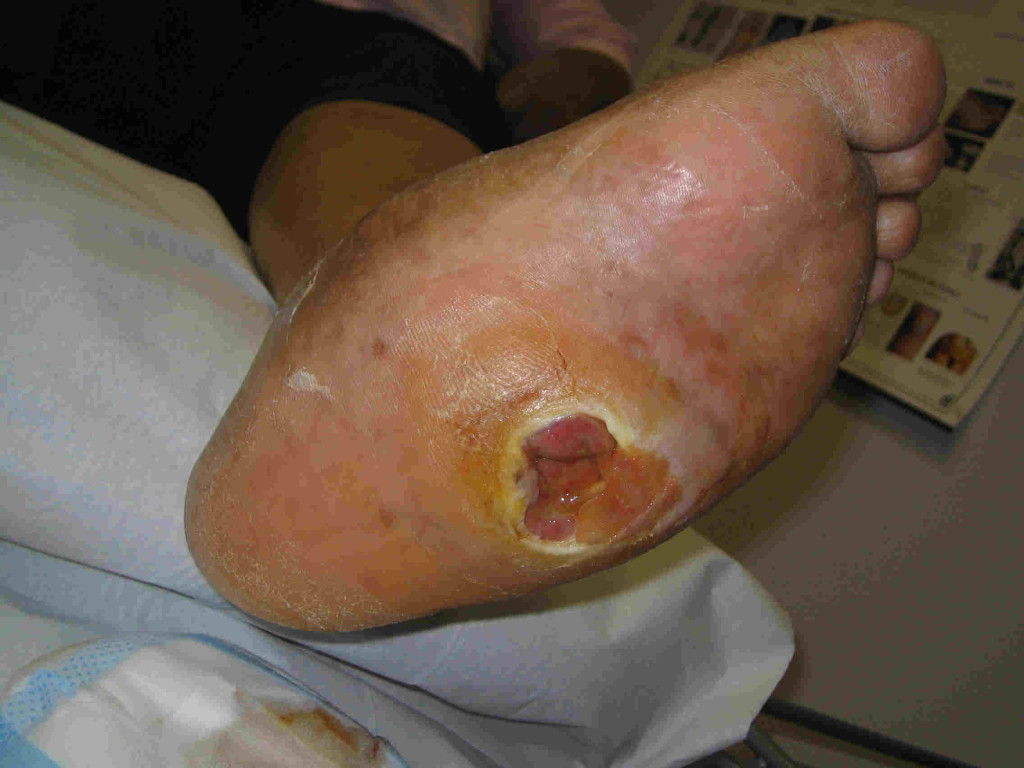
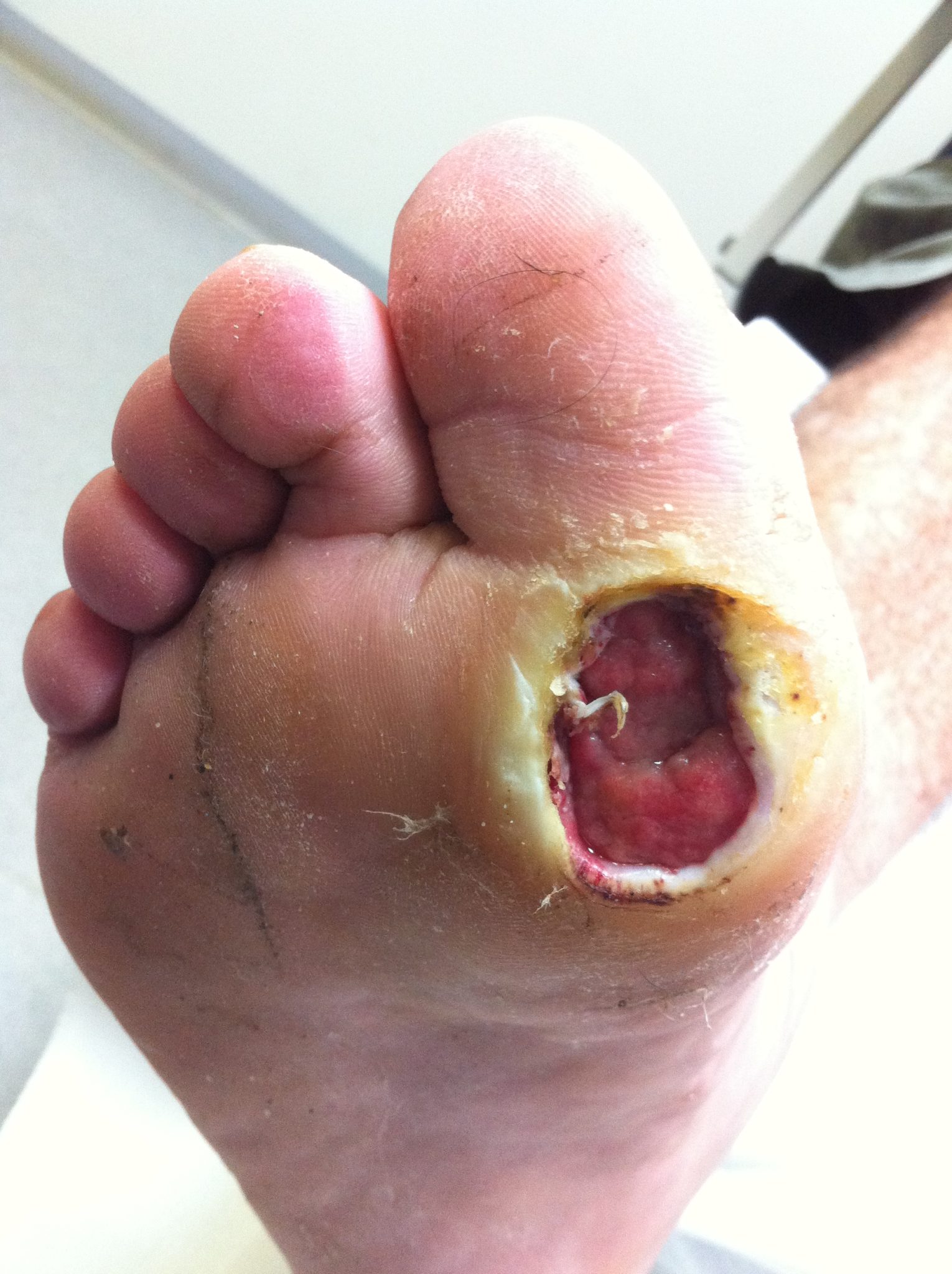
Foot Ulcers
Foot ulcers are an undesirable complication of either peripheral neuropathy and/or peripheral arterial disease. These wounds can be difficult to heal unless a good understanding of the cause of the problem is taken into consideration.
Most typically, neuropathic foot ulcers are painless wounds under the joints of the front of the foot, or around the toes. They are primarily caused by unremitting pressure over bony prominences, altered biomechanics, and the lack of ability to feel pain. If blood flow is still good, they are usually relatively easy to heal once suitable pressure offloading is done with either special footwear, orthotics, bracing or casts. There is usually a preponderance of hyperkeratotic tissue (hard skin callus) around the wound, along with non-viable tissue that needs removal by surgical debridement. This is thankfully painless and promotes much more rapid healing.
The use of special dressings to heal these wounds is typically not of great importance, and simple sterile dressings are usually sufficient because the focus is on removing pressure from these areas.
Our podiatrists will need to see the wound regularly for wound debridements, and to evaluate the effectiveness of pressure offloading approaches.
By contrast, ischaemic ulcers are due to a lack of blood supply (caused by peripheral arterial disease) reaching the foot, and necrosis of the skin following often trivial injury. They are far more difficult to heal unless restoration of blood flow to the foot can be achieved. We will often work with your GP and vascular surgeon to look for ways to get better blood flow back into the foot, in order for these to heal. It may be important to use protective footwear or bracing during this period to protect these fragile tissues from any further pressure or injury.